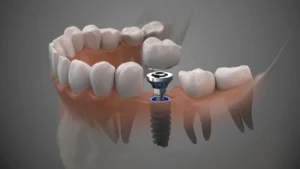
Eating after dental implant surgery is often more challenging than people expect. Even when pain feels manageable, swelling, tenderness, and limited jaw movement can make everyday meals uncomfortable. Many people find themselves less focused on taste and more concerned about choosing foods that won’t disturb the healing area.
During recovery, food choices are not only about comfort. Certain textures can place pressure on healing gums, interfere with the blood clot that protects the surgical site, or slow the body’s natural repair process. At the same time, your body still needs steady nutrition to support tissue repair and bone healing.
This guide explains how eating typically changes after implant surgery, what food textures are often easier at different stages of recovery, and examples of 50 soft foods to eat after dental implant surgery that many patients tolerate well. Understanding when to adjust food textures can help reduce discomfort and support a smoother healing process.
Why Food Choices Matter During Implant Recovery
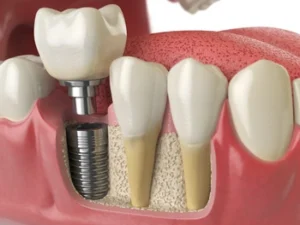
Foods that require strong biting or grinding can shift pressure toward the healing site. This can irritate the surrounding tissues or interfere with the natural protective process that takes place immediately after surgery. Choosing softer foods helps limit unnecessary movement in the area while still allowing your body to receive the nutrients it needs.
Soft foods are generally easier to manage when the mouth feels tender or swollen. They reduce chewing effort, are simpler to swallow, and allow healing to progress without placing extra strain on the implant area.
Choosing Foods That Match Your Healing Stage
Comfort and tolerance often change as healing progresses. Early on, eating is less about variety and more about minimising effort while meeting basic nutritional needs. As swelling reduces and movement becomes easier, food texture can gradually change to match what feels manageable.
In the first few days, liquids and very soft foods are usually easier to handle, as they require little jaw movement. As recovery continues, slightly thicker or more textured foods can be introduced in stages, provided they do not cause discomfort or require heavy chewing.
Many people find the following options easier during recovery:
- Soft, mashed foods that provide energy without chewing strain
- Gentle protein sources that support tissue repair
- Blended or pureed vegetables for added nutrients
- Moist, tender foods once chewing becomes more comfortable
- Smooth drinks that help maintain nutrition when appetite is reduced
Food choices should always be guided by comfort rather than a fixed timeline.
Foods That Can Interfere With Healing
During recovery, sensitivity can be affected by how foods behave in the mouth, not just how firm they are. Heat, acidity, texture, and chewing effort all play a role in how comfortable eating feels while tissues are still settling.
It generally helps to limit:
- High-temperature foods and drinks, as excessive heat can increase tenderness and disrupt early healing
- Citrus-based and tomato-based liquids, which may cause stinging or irritation around healing tissues
- Foods that require prolonged chewing, such as dense meats, sticky sweets, or thick bread edges, which can strain the surgical area
- Hard or brittle foods, including crisp snacks or toasted items, that may press against sensitive sites
- Strongly seasoned foods, particularly those containing chilli or similar spices, which can irritate healing gums
- Foods that combine heat and acidity, as this combination may heighten discomfort during recovery
As healing progresses and comfort improves, these foods can usually be reintroduced gradually with guidance from your dentist.
50 Soft Foods to Eat After Dental Implant Surgery
During implant recovery, different stages of healing call for different food textures. Organising soft foods by recovery phase helps reduce strain on the surgical site while still supporting nutrition, comfort, and energy levels.
First 48 Hours: No-Chew & Spoon-Soft Foods
These foods require minimal jaw movement and are best tolerated immediately after surgery.
- Broth-based soups
- Soups (lukewarm, not extremely hot)
- Protein shakes or meal replacement drinks
- Protein powder mixed with milk
- Smoothies (avoid seeds)
- Yoghurt (plain or Greek)
- Yoghurt smoothies with added vitamin C-rich fruits
- Applesauce
- Jelly
- Custard
- Pudding
- Blended fruit (non-acidic)
- Chia pudding (soaked well)
Days 3–5: Gentle Energy & Soft Proteins
As swelling reduces, soft protein sources support tissue repair without placing stress on the implant site.
- Scrambled eggs
- Poached eggs
- Egg salad
- Cottage cheese
- Tofu
- Baked beans
- Refried beans
- Hummus
- Tuna salad (mashed finely)
- Ground turkey
Days 5–7: Comfort Carbohydrates
Soft, filling foods that provide energy, as chewing comfort improves.
- Mashed potatoes
- Sweet potatoes
- Mashed peas
- Pureed pumpkin
- Vegetable mash
- Steamed vegetables (soft and well-cooked)
- Polenta
- Rice pudding
- Cream of wheat
- Oatmeal
- Porridge
- Cooked oats with milk
- Bananas (ripe and soft)
Week 2 and Beyond: Soft Chew Foods (With Care)
Only introduce these foods once approved by your dentist.
- Soft fish (such as salmon or cod)
- Shredded chicken (moist and tender)
- Well-cooked pasta
- Rice noodles
- Creamy risotto
- Macaroni and cheese
- Quiche
- Pancakes
- Soft muffins (without nuts or seeds)
- Soft bread (no crusts)
Long-Term Soft Staples
Suitable if healing takes longer or chewing remains uncomfortable.
- Avocado mash
- Smooth peanut butter
- Lentil soup
- Creamy soups (such as potato or pumpkin)
Eating Habits That Support Implant Healing
Eating well is key to helping your body heal and stay strong. Here are a few practical tips to follow during recovery:
- Increase protein intake: Protein helps your tissues repair faster and keeps you full. Try adding protein powder to smoothies or milk for an easy boost.
- Include vitamin C: Vitamin C-rich foods such as mashed sweet potatoes or smooth fruit purees support gum healing and ease inflammation.
- Keep hydrated: Have plenty of water, but steer clear of hot drinks or acidic juices while your gums are still sensitive.
- Avoid spicy foods: Spices and strong flavours can irritate the healing gum tissue.
- Try meal replacements: If chewing feels difficult, blended smoothies or shakes can help maintain your protein intake and overall nutrition.
Transitioning Back to Firmer Foods
After the first week, your dentist may suggest reintroducing more solid foods, depending on how your healing process is going. As part of what to do after dental surgery, start with soft, tender meals such as pasta, fish, or shredded chicken before moving on to chewy foods or crunchy foods.
Avoid biting directly on the surgery site until your dentist says it’s safe. It can take several weeks for your implant area to fully stabilise, especially if you had multiple dental implants, a regular tooth extraction, or a wisdom tooth extraction during the same procedure.
Soft Food Considerations if Healing Takes Longer
If your healing phase takes longer, it’s okay to continue a soft food diet for a little longer. You can mix up your meals with soups, mashed potatoes, or other soft foods to prevent boredom. Avoid foods that are extremely hot, spicy, or acidic to keep your surgical site comfortable and healing well.
Common Questions Patients Ask During Implant Recovery
Patients often ask these questions as eating comfort changes during healing.

Yes. Even when discomfort is minimal, the tissues around the implant are still healing beneath the surface. Continuing with soft foods for the recommended period helps avoid unnecessary pressure while the implant stabilises.
Why does chewing on one side feel easier at first?
Many people naturally avoid the surgical side during early recovery. This is a normal protective response. As tenderness reduces and your dentist confirms healing is progressing well, balanced chewing usually becomes more comfortable again.
Is it normal for certain soft foods to still feel uncomfortable?
It can be. Sensitivity levels vary, and some textures may feel irritating even if they are considered soft. If discomfort persists or worsens, it’s best to pause that food and choose alternatives that feel more comfortable.
When should I contact the clinic about eating discomfort?
If pain increases, swelling does not continue to improve, or eating remains difficult beyond the expected healing timeframe, it’s important to check in with your dentist for advice.
Consistency and Care During Ongoing Recovery
Recovery after dental implant surgery doesn’t follow the same timeline for everyone. Some people find eating becomes comfortable within days, while others notice tenderness or sensitivity that lasts longer. Paying attention to how different food textures feel, rather than rushing back to normal meals, can help reduce unnecessary pressure on the implant site.
If discomfort increases, chewing remains difficult, or swelling does not continue to improve, it’s best not to ignore these signs. Ongoing sensitivity can indicate that adjustments to eating habits or recovery care are still needed.
If you’d like guidance on food choices during your recovery or have concerns about how healing is progressing, you’re welcome to book a consultation with us at Balmoral Dental Centre or call (07) 3113 9789 to speak with our team.
Resources
Cleveland Clinic Staff. (2024). ‘What To Do After Oral Surgery: Recovery and Self-Care’. Cleveland, OH, 5 July. Cleveland, OH: Cleveland Clinic.
https://health.clevelandclinic.org/post-op-recovery-oral-surgery
Kubala, J. (2023). ‘Soft Food Diet: Foods to Eat and Foods to Avoid’. New York, NY, 15 March. New York, NY: Healthline Media.
https://www.healthline.com/nutrition/soft-food-diet
Note: Any surgical or invasive procedure carries risks. Before proceeding, you should seek a second opinion from an appropriately qualified health practitioner.